Educational consequences of teenage pregnancy Teenage pregnancy is a world disaster, and it has...
Sexually Transmitted Infections
Sexually Transmitted Infections
An STI is an infection spread predominantly by sexual contact, including kissing, vaginal, anal and oral sex.
Quick Links
STI Screening
Bacterial STI
Viral STI
Herpes
Human Papillomavirus
Hepatitis
HIV
Parasitic STI
Trichomoniasis
Pubic Lice
Fungal STI
Yeast Infection(Vaginal)
Yeast Infection(Penile)
What is it?
- An STI is an infection spread predominantly by sexual contact, including kissing, vaginal, anal and oral sex. Some STIs can also be transmitted from mother-to-child during pregnancy, childbirth and breastfeeding. An infection is when a bacteria, virus, or parasite enters and grows in or on your body. STIs are also called sexually transmitted diseases, or STDs.
- More than 30 different bacteria, viruses and parasites are known to be transmitted through sexual contact. Eight of these pathogens are linked to the greatest incidence of sexually transmitted disease. Of these, 4 are currently curable: syphilis, gonorrhea, chlamydia and trichomoniasis. The other 4 are viral infections which are incurable: hepatitis B, herpes simplex virus (HSV or herpes), HIV and human papillomavirus (HPV).
- A person can have an STI without showing symptoms of disease. Common symptoms of STIs include vaginal discharge, urethral discharge or burning in men, genital ulcers and abdominal pain.
- Common STDs in women include Chlamydia, genital herpes, human papillomavirus (HPV) infection, syphilis, gonorrhea, pubic lice, chancroid, and HIV/AIDS.
STI Screening
STI tests are relatively easy and depending on the type of STI test, could range from 20 minutes to a week for results.
Based on Common Types of Tests
For both
- Check your genitals visually
- Take a swab from a wound or sore
- Ask for a urine sample
- Take a blood test
For women
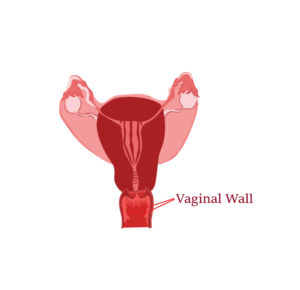
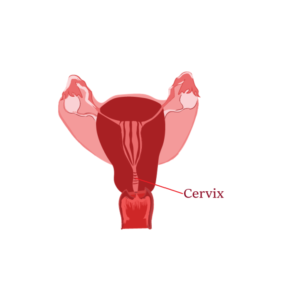
- Inspect vaginal walls and cervix
- Swab from your vagina and/or cervix
For men
- Touch your penis and testicles to check for discharge, pain or sores Take a swab from your urethra (opening of the penis)
Based on the type of STI
- Vaginitis: Pelvic exam (look inside your vagina for inflammation and abnormal discharge) and pH testing
- Chlamydia & Gonorrhea : Swab of genital area, urine sample
- Syphilis: Blood test, sample from a sore
- Pelvic Inflammatory Disease: Pelvic exam, blood, test, urine test, ultrasound, laparoscopy (inserts a thin device through a small cut in your abdomen to view pelvic organs), endometrial biopsy (inserts a thin tube into the uterus to sample endometrial tissue for signs of infection & inflammation)
- Genital Herpes
- No symptoms: Blood test
- With symptoms: Swab of infected area and blood test
- Human Papillomavirus (HPV): HPV test (women), visual exam. There is currently no approved test for HPV in men however, visit your doctor immediately if you notice any abnormal skin growths or changes in your penile, scrotal, anal, or throat areas.
- Hepatitis B & C: Blood tests
- Human Immunodeficiency Virus (HIV): Blood, oral fluid and urine test
- Trichomoniasis: Swab of infected area, visual exam or a sample of discharge
- Pubic Lice: skin exam
- Yeast Infection (Vaginal): Pelvic exam, sample of vaginal fluid
Yeast Infection (Penile): swab of infected area, blood and urine test
Get vaccinated – There are vaccines to protect against HPV and hepatitis B.
Use condoms – Condoms are the best way to prevent STIs when you have sex. Condoms can protect against some, but not all, STDs and are never 100% effective in protecting against STDs. Other birth control methods, like birth control pills, shots, implants, or diaphragms, will not protect you from STIs.
Do not douche –Vaginal douching is washing the vagina with a mixture of fluids such as vinegar, baking soda or iodine. A few also contain antiseptics and fragrances. It can cause side effects like burning and irritation. Douching removes some of the normal bacteria in the vagina that protects you from infection. This may increase your risk of getting STIs.
- Bacterial STDs such as chlamydia, syphilis, and gonorrhea can be cured by antibiotic treatment.
- No cure is available for some STDs like HIV or chronic hepatitis B infection, but medications are available to manage these chronic conditions.
- The pelvic inflammatory disease (PID) and infertility are complications of some STDs. Other complications depend upon the specific type of illness.
Educational consequences of teenage pregnancy
Biological and psychosocial changes during adolescence
Biological and psychosocial changes during adolescence The most important psychological and...
Diabetes Mellitus and its complications on SRH
Diabetes Mellitus and its complications on SRH Diabetes is a chronic metabolic disease that is...
Somatization and SRH
Somatization and SRH Somatization disorder or somatic symptom disorder is a chronic condition...
Cognitive disorders and SRH
Cognitive disorders and SRH Cognitive disorders are a part of the neurocognitive disorder...
Bacterial STIs
Bacterial STIs/STDs are caused by bacteria, tiny single-celled microorganisms. Bacteria are highly resistant and are able to survive in various environments. Our body is home to many microorganisms and not all of them are dangerous.
Since bacterial STIs/STDs often give no warning signs, you can contract and transmit it without your knowledge. This means that before you realize the problem, serious complications which can cause irreversible damage can progress silently.
They are curable through treatment with antibiotics as long as you get tested and treated, follow through on all the medication, avoid sexual contact until cured, and make sure your sexual partner(s) get tested and treated as well.
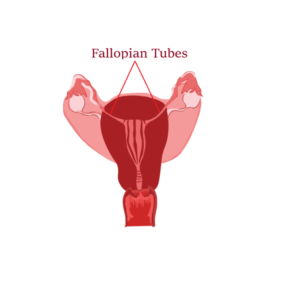
Complications can include pelvic inflammatory disease, urethritis, infertility, and ectopic pregnancy (a pregnancy in which the fetus develops outside the uterus, typically in a fallopian tube). The longer it is left untreated, the more damage it can do. Medication will stop the infection, but it will not repair any permanent damage done before treatment begins.
Vaginitis
Vaginitis, also called vulvovaginitis, is an inflammation or infection of the vagina and can also affect the vulva, which is the external part of a woman’s genitals. Vaginitis can cause itching, pain, discharge, and odor.
Common Cause
Bacterial vaginosis (BV) is the most common vaginal infection in women ages 15-44. It occurs when there is an imbalance between the “helpful” and “harmful” bacteria typicallyouter found in a woman’s vagina.
Several things can change the balance of bacteria, such as taking antibiotics, douching, using an intrauterine device (IUD), having unprotected sex with a new partner, or having many sexual partners.
Another cause for vaginitis is yeast infections (candidiasis), typically outer when too much candida grows in the vagina. Candida is the scientific name for yeast that lives naturally in your mouth, gut, and vagina.
You may have too much growing in the vagina because of antibiotics, pregnancy, diabetes, especially if it is not well-controlled, corticosteroid medicines.
Trichomoniasis can also cause vaginitis. It is a common sexually transmitted disease caused by a parasite.
You can also have vaginitis if you are allergic or sensitive to certain products that you use. Some products that can cause burning, itching, and discharge are vaginal sprays, douches, spermicides, soaps, detergents, or fabric softeners.
You can have more than one cause of vaginitis at the same time. Therefore, it is essential to treat BV and trichomoniasis because having either can increase your risk of getting HIV or another sexually transmitted disease. BV or trichomoniasis can increase your risk for preterm labor and preterm birth if you are pregnant.
Symptoms
Bacterial vaginosis: have a thin white or gray vaginal discharge with an odor, such as a strong fish-like odor, especially after sex.
Yeast infections: produce a thick, white discharge from the vagina that can look like cottage cheese. It can be watery, often has no smell, and usually causes the vagina and vulva to become itchy and red.
Trichomoniasis: you may not have symptoms, but if you do, you could have gray-green discharge, which may smell bad. You can also have itching, burning, and soreness of the vagina and vulva.
Treatment
Bacterial vaginosis: is treatable with antibiotics. You may get pills to swallow or cream/gel to apply in your vagina. You should use a condom or not have sex until you are cured.
Yeast infections: are usually treated with a cream or medicine that you put inside your vagina. You can buy over-the-counter treatments for yeast infections, but you need to be sure that you do have a yeast infection, so you must see your doctor for a diagnosis. Even if you have had yeast infections before, double-checking is a good idea.
Trichomoniasis: treatment is usually a single-dose antibiotic that you and your partner(s) take to prevent spreading to others and avoid getting it again.
Allergy or sensitivity to a product: find out which product is causing the problem and stop using the product.
Hormonal change: consult your doctor, who may give you estrogen cream to help with your symptoms.
Prevention
- Do not douche or use vaginal sprays.
- Use a latex condom when having sex. If your partner is allergic to latex, you can use polyurethane (type of plastic) condoms.
- Avoid clothes that hold in heat and moisture
- Wear cotton underwear
Chlamydia
Chlamydia is a common STD that can cause serious, permanent damage to a woman’s reproductive system. This can make it difficult or impossible to get pregnant later on. Chlamydia can also cause a potentially fatal ectopic pregnancy (pregnancy that occurs outside the womb). It can be easily cleared up with antibiotics. But if you don’t treat chlamydia, it may lead to major health problems in the future.
Common Cause
The bacterium Chlamydia trachomatis causes chlamydia. It commonly affects 14-24-year-old and be contracted during oral, vaginal, or anal sex with someone who has the infection. A woman can also pass chlamydia to her baby during childbirth or by carrying the infected liquid on hands to the eyes, which is rare. If you’ve had chlamydia and were treated in the past, you can get re-infected if you have unprotected sex with someone who has it.
Chlamydia can’t be spread through casual contact, so you are safe from infection even if you share food or drinks, kiss, hug, hold hands, cough, or sneeze. The best way to prevent infection is by using condoms orher dental dams (a thin, flexible piece of latex that protects against oral sex) every time you have sex.
Symptoms
Chlamydia often runs without symptoms, making it potentially dangerous, especially for women’s fertility.
Sometimes this disease shows up through:
- unusual discharge from the genitals
- sometimes yellowish and smelly painful urination
- bleeding during or after the intercourse
- bleeding between periods or heavy periods
- pain in the lower abdominal sometimes with nausea and low-grade fever
- swollen skin inside the vagina or around the anus
- If chlamydia infects your eyes, you may have redness, skin discoloration around your eye, itching, or discharge. Sometimes chlamydia infections in the throat cause soreness, but it’s rare.
Treatment
Chlamydia is effectively treated with antibiotics if diagnosed early, but it cannot repair any permanent damage that the disease has caused. Your doctor will help you figure out which treatment is best for you. Depending on the severity, you may only have to take one dose or several that last seven days.
To prevent spreading the disease, you should wait seven days after taking the single dose or until you finish taking all the doses for seven days. Your partner(s) should also get treated to prevent infecting others or re-infecting each other. It is common to get a repeat infection, so you should get tested again about three months after treatment.
If left untreated for a long time, it can spread to your uterus and fallopian tubes, causing pelvic inflammatory disease (PID). This can cause permanent damage that leads to pain, infertility, or ectopic pregnancy. Therefore, regular checkups are necessary to lower your chances.
Prevention
- Abstain from sex contacts or limit the number of sex partners
- Use condoms during every intercourse
- Make sure your new sexual partner is uninfected (encourage them to get tested) o
- Avoid using water-based spermicides.
- Get tested regularly if you have active sexual life and often change partners.
Gonorrhea
Gonorrhea is an STI most common in young adults. Gonorrhea is an STI very similar to chlamydia in the way it is transmitted and the way it is treated. Gonorrhea mostly attacks the urethra, cervix, and fallopian tubes.
It has a nickname called the clap because it refers to a treatment that is used to clear the blockage in the urethra from gonorrhea pus, where the penis would be ‘clapped’ on both sides simultaneously.
The bacteria grow in warm, moist areas of the body and can include the urethra (the tube that carries urine out of the body) and grow in the eyes. It is an especially serious problem for women because it can damage the female reproductive organs (the fallopian tubes, uterus, and cervix).
Common Cause
Gonorrhea is caused by Neisseria gonorrhoeae and can infect the genital tract, mouth, or anus. You can get gonorrhea during vaginal, oral, or anal sex with an infected partner. A pregnant woman can pass it to her baby during childbirth. Gonorrhea most often affects women ages 15 to 24 but is becoming more common in older women.
Symptoms
This disease can show no symptoms in most women, but sometimes signs are noticeable.
- bleeding between periods
- pain when urinating
- increased discharge from the vagina.
- If untreated, it can lead to pelvic inflammatory disease, which causes problems with pregnancy and infertility.
- Rectal infections may either cause no symptoms or cause symptoms that may include discharge, anal itching, soreness, bleeding, and painful bowel movements.
Treatment
The patients with chlamydia are almost always prescribed to take medications against gonorrhea and vice versa. The antibiotics are usually a pill you swallow. Although antibiotics can cure gonorrhea, they cannot fix any permanent damage done to your body. For this reason, it is essential to get tested and take antibiotics immediately.
To be cured, you must finish all antibiotics even if the symptoms go away and do not share your antibiotics with anyone. See your doctor if symptoms do not go away after treatment. It is possible to get reinfected if you have sex with someone who has gonorrhea. You should inform your recent sex partner(s), so they can be tested and treated as well.
Gonorrhea that is not treated can cause serious health problems in women, such as pelvic inflammatory disease (PID), leading to chronic pelvic pain, pregnancy problems, and infertility. It can also put you at a higher risk of getting HIV or spreading HIV. Although it is not common, gonorrhea can cause widespread infection in other parts of the body (blood, joints, heart, or brain) and can lead to death.
Prevention
Your content goes here. Edit or remove this text inline or in the module Content settings. You can also style every aspect of this content in the module Design settings and even apply custom CSS to this text in the module Advanced settings.
Syphilis
Syphilis is one of the most common sexually transmitted diseases (STDs). It is a bacterial infection spread through vaginal, oral, or anal sex with an infected person. Syphilis develops in stages that can last for weeks, months, or even years. The stages may be separated by long periods of apparent good health. It usually starts with a small, painless sore, called a chancre, on the genitals, anus, or mouth. In the next stage, you may have flu-like symptoms and/or a rash. Later stages of syphilis can damage the brain, heart, spinal cord, and other organs.
Common Cause
Syphilis is a disease caused by the bacterium Treponema pallidum. Young adults ages 20 to 35 are usually the highest at risk of getting this disease. This bacterium causes infection during sexual activity but can also get into your body through cuts on your skin or through your mucous membranes. Syphilis is most often transmitted through sexual contact with someone who has it. It can also pass from mother to baby during pregnancy.
It can’t be spread by toilet seats, doorknobs, swimming pools, hot tubs, bathtubs, shared clothing, or eating utensils.
Symptoms
Sometimes syphilis is difficult to distinguish as it can imitate the course of other diseases, but generally, it starts with the sore in the area of the penis or vagina. If you do not treat it, syphilis usually causes a non-itchy skin rash, often on your hands and feet. Many people do not notice symptoms for years. Symptoms can go away and come back.
The sores caused by syphilis make it easier to get or give someone HIV during sex. If you are pregnant, syphilis can cause complications, or you could lose your baby. In rare cases, syphilis causes serious health problems and even death.
Syphilis is divided into stages (primary, secondary, latent, and tertiary), with different signs and symptoms associated with each stage.
Primary syphilis: occurs between 10 and 90 days (3 weeks on average) after you’re exposed to the disease. It causes one or more sores called chancres on or around the genitals, around the anus or in the rectum, or in or around the mouth. These sores are usually firm, round, and painless. Even if you don’t treat them, they heal without a scar within six weeks. But treatment will keep your disease from moving to the next stage.
Secondary syphilis: begins six weeks to 6 months after you’re exposed and can last 2 to 6 weeks at a time and may come and go for up to 2 years. Symptoms include a pinkish rash on the palms, soles of the feet, and on other parts of their body. The inflammation is sometimes hard to see, and it usually doesn’t itch.
People may have moist, wart-like lesions in their groin, white patches on the inside of their mouth, swollen lymph glands, fever, hair loss, and weight loss.
The signs and symptoms of primary and secondary syphilis can be mild, and they might not be noticed. As with primary syphilis, symptoms of secondary syphilis will get better without treatment.
Latent stage: there are no signs or symptoms for months or even years, but you still need treatment to get rid of it.
Tertiary syphilis: isn’t contagious at this point, but the infection has started to affect your organs. It can cause tumors, blindness, and paralysis, damage your nervous system, brain, and other organs, and even kill you.
The damage that late-stage syphilis has already caused can’t be changed or healed. The complications from late-stage syphilis can happen 10-20 years after you first get infected.
Treatment
Syphilis is easy to cure with antibiotics if you catch it early. A blood test is a reliable way to detect this disease, and the preferred treatment at all stages is the antibiotic penicillin. To get cured, you might only need one injection of penicillin if you’ve been infected for less than a year and more doses if it’s more than a year.
After getting a penicillin injection or taking other antibiotics, you may experience fever, headaches, joint or muscle pain, all of these in addition to nausea and chills. These usually only last about a day. There are no over-the-counter medications or home remedies that will cure syphilis — only antibiotics can do that.
Your sexual partner(s) needs to get treated to prevent transferring to other people and back to each other. You should abstain from sex until you finish your treatment and all the sores are have healed.
Prevention
- Not have vaginal, anal, or oral sex.
- Have a mutually monogamous relationship with a partner who has been tested and is clean
- Correct usage of latex condoms significantly reduces (but does not eliminate) the risk of catching or spreading. If you or your partner is allergic to latex, you can use polyurethane (type of plastic) condoms.
Pelvic Inflammatory Disease
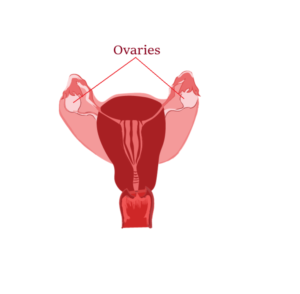
Pelvic Inflammatory Disease (PID) affects only women and comes as a result of bacteria moving from vagina or cervix to the uterus, fallopian tubes, ovaries, or pelvis. It causes scarring in these organs and can lead to infertility, ectopic pregnancy (a complication of pregnancy in which the embryo attaches outside the uterus), pelvic pain, abscesses, and other serious problems.
Common Cause
Gonorrhea and chlamydia are two STDs that commonly cause PID. It can develop as the complication of these two STDs, which damage the fallopian tubes and tissues in and around the uterus and ovaries and might also lead to infertility in severe untreated cases. Other causes include abortion, childbirth, pelvic procedures, and an intrauterine device (IUD), either copper or hormonal. You are more likely to get infected if you are younger than 25 and sexually active (one or more partners) and if you douche.
Symptoms
Some women have no symptoms. Others have:
- Pain in the lower abdomen
- Fever
- Smelly vaginal discharge
- Irregular bleeding
- Pain during intercourse or urination
Treatment
PID is easily cured with antibiotics taken orally if caught early on. However, late detection can have harmful consequences to the reproductive system that can be irreversible and increase the risk of infertility.
To fully treat PID, you may need to take one or more antibiotics to clear the infection in about two weeks. You should take it simultaneously every day and finish all of it even if you feel better. The infection can come back if you do not quit. Your doctor will inform you what types of foods, alcohol, or other medicines you should avoid until you finish the treatment.
You and your sexual partner(s) must be treated to prevent PID from coming back. Use condoms until you both(all) have finished taking antibiotics.
These antibiotics can have side effects such as:
- Nausea
- Diarrhea
- Stomach pain
- Rash and itching
- Vaginal yeast infection
Prevention
- Practice abstinence
- Having a sexual relationship with only one person
- Using a condom every time you have sex
- Get regular checkups
Viral STIs
Viral STDs are caused by viruses that dwell inside a person. Viral infections spread by modifying human cells and producing more viral cells. Viral STDs usually have no symptoms. If they do, the symptoms like sores or blisters for genital herpes come and go making it easy to get infected and transmit unknowingly.
You can get this disease even if you are not sexually active. It can be transmitted during blood transfusion, pregnancy, birth, breastfeeding, and sharing personal things such as towels or toothbrushes.
There is no permanent cure for viral STDs, and many can persist for a long time. It could go on for your whole life and could bring irreversible damage to your health if left untreated. This is why early treatment can keep it managed for a continuous period, relieve symptoms, and minimize the impact on the patient’s day-to-day life. In addition to this, there are vaccines to help prevent HPV and hepatitis. Until the active treatment is finished, it is vital to abstain from sex.
Herpes
Herpes is a common infection that stays in your body for life. It causes sores on your genitals or mouth. Herpes can be annoying and painful, but it usually doesn’t lead to serious health problems.
Common Cause
Two different but similar viruses cause herpes:
- Herpes simplex virus type 1 (HSV-1): causes oral herpes, which usually affects the mouth and surrounding skin.
- Herpes simplex virus type 2 (HSV-2): causes genital herpes, usually sexually transmitted.
It is spread through contact with the infected parts of the skin, mainly during intercourse, but in some cases, it can be transmitted from mother to child while giving birth. It can also be spread by direct contact of the skin by blistered areas, but transmission can also happen even if there are no outbreaks.
Symptoms
The first symptoms to develop are tingling, itching, or burning, and then you might notice sores or blisters forming around the mouth or genitals. It takes 2–20 days to develop these symptoms after exposure to the virus.
Oral Herpes
- Oral herpes usually is less painful than genital herpes and. Symptoms can fade away and pop up again in weeks, months, or years. They are typically harmless in kids and adults but can be dangerous to newborn babies.
Symptoms include:
- Sores in or around your mouth are referred to as cold sores or fever blisters that last a few weeks and fo away on their own
Genital herpes
It’s called an outbreak when blisters and other genital herpes symptoms show up. The first outbreak usually starts about 2 to 20 days after you get infected, getting infected, getting but sometimes it takes years for the first outbreak to happen.
The first outbreak lasts about 2 to 4 weeks, getting infected, and even though the blisters go away, the virus stays in your body and can cause sores again. It’s really common to get repeat outbreaks, especially during the first year you have herpes.
Symptoms include:
- Several itchy or painful blisters (vagina, vulva, cervix, anus, butt, or the inside of your thighs). These blisters then break and turn into sores.
- Burning when you pee if your urine touches the herpes sores or if it is blocking your urethra (the tube that passes from the bladder to the outside of the body).
- Fever, chills
- Headache
- Feeling achy and tired
Treatment
Although herpes symptoms are easy to treat, there’s no cure against the virus, so that that infected people will have it for the rest of their lives. After the outbreak lasts 2–3 weeks, the disease goes into a dormant stage, with the infected person remaining a potential transmitter. However, some people never develop symptoms.
No drug can get rid of the herpes virus. However, a doctor may prescribe an antiviral medication, such as acyclovir, to prevent the virus from multiplying. There are also over-the-counter herpes treatments, usually creams, to help manage tingling, itching, and pain.
If a person uses antiviral medication, symptoms may resolve 1–2 days more quickly than if they had used no treatment and may lessen the severity of symptoms. Depending on the frequency of recurrence, a doctor may recommend you to take medication for 6-12 months at a time. You can reduce the likelihood of transmitting by taking these medications every day for longer periods.
Prevention
- Using barrier protection, such as condoms and dental dams, when having sex
- Avoiding sex while symptoms are present
- Avoiding kissing and oral sex when there is a cold sore around the mouth
- Washing the hands thoroughly, especially after touching the affected area, during an outbreak
Human Papillomavirus
Human Papillomavirus (HPV), also known as “genital warts’ ‘ is a widespread disease with about 100 types detected. It passes from person to person through sexual contact, primarily through skin-to-skin contact with the infected areas. Warts are highly contagious, but even the dormant stage without warps can infect other people.
Common Cause
HPV infection is caused by HPV, a type of the Papillomaviridae strain. HPV-6 or HPV-11 are usually the ones that cause genital warts. There are high-risk HPV that are even more serious and can cause cancer in the reproductive systems of both men and women.
The virus that causes HPV infection is transmitted through skin-to-skin contact. You can get a genital HPV infection through direct sexual contact, including vaginal, anal, and oral sex.
Since many people don’t get symptoms, they contract and spread them, but it is possible to have multiple HPVs without being aware. A mother can transmit the virus during delivery which might cause the baby to develop a condition called recurrent respiratory papillomatosis (HPV-related warts inside the throat or airways).
Symptoms
Most people do not experience any symptoms of HPV, and the virus often goes away by itself. But in some people, HPV causes.
- Genital warts
- Cancer
- Pain during sex
- Bleeding after sex
- Abnormal periods, unusual vaginal bleeding, or unusual discharge
- Itchiness
- Pain in the pelvis
Treatment
There is no treatment for HPV; however, the body usually gets rid of the virus by itself over the course of a year. To make sure it is gone, you need to be re-tested. Even if warts no longer occur, it is necessary to undergo regular checkups to prevent HPV from developing into cancer.
If you develop genital warts, your doctor may suggest:
- Cryotherapy: using liquid nitrogen to freeze off warts
- Electrocautery: an electrical current to burn away the warts
- Laser or light therapy: using a high-powered, targeted beam to remove the unwanted tissue
- Surgical removal: cut away the warts
Prevention
- Using condoms is necessary, but you can still catch HPV because the whole genital area isn’t covered.
- A vaccine is available that can protect against nine types of HPV known to be associated with either cancer or genital warts.
- Get regular health checkups, screenings, and Pap smears.
Hepatitis
Hepatitis means inflammation of the liver, which affects the function of the liver. There are several causes for hepatitis, such as heavy alcohol use, toxins, medications, and certain medical conditions. Usually, hepatitis is caused by a virus. The most common hepatitis viruses are hepatitis A virus (not commonly sexually transmitted), hepatitis B virus, and hepatitis C virus (not commonly sexually transmitted).
Hepatitis B
Hepatitis B is the most common severe liver infection globally that attacks and injures the liver. Most people do not have symptoms when they are newly or chronically infected and can unknowingly spread the virus to others.
Common Cause
The hepatitis B virus causes hepatitis B. Some people with hepatitis B are sick for only a few weeks, known as acute hepatitis B. Still, for others, the disease progresses to a severe and lifelong illness known as chronic hepatitis B.
Hepatitis B is a sexually transmitted virus spread through the infected blood, semen, and vaginal fluids that cause the inflammation of the liver. It can also be applied by:
- An infected mother to her baby during birth
- Sharing needles, syringes, or drug preparation equipment
- Sharing items such as toothbrushes, razors, or medical equipment (like a glucose monitor) with an infected person
The chance of developing chronic infection is more significant when a a person is (0-6 years old). Children older than six years old and adults recover completely and do not develop chronic infection.
Symptoms
Most people do not experience any symptoms when newly infected. However, some people have acute illness with symptoms that last several weeks, such as:
- Flu-like symptoms like nausea, tiredness, loss of appetite, and muscle pain
- Yellowing of the skin and eyes (jaundice)
- Dark urine
- Vomiting
- Abdominal pain.
- Can develop acute liver failure, which can lead to death
Treatment
There’s no cure for hepatitis B, but there’s an effective vaccine that can help prevent this dangerous disease. Therefore, you need to maintain comfort and adequate nutritional balance, such as substituting fluids lost from vomiting and diarrhea. You must avoid unnecessary medications such as acetaminophen, paracetamol, and medication against vomiting.
The infection can be treated with medicines, including oral antiviral agents, which can slow the advancing of complications and improve long-term survival.
Prevention
-
Getting vaccinated is the best way to prevent hepatitis B. Other methods include:
- Implementation of blood safety strategies
- Safer sex practices (limit the number of partners and using barrier protective measures like condoms)
Hepatitis C
Hepatitis C is a virus that can infect the liver. If left untreated, it can sometimes cause severe and potentially life-threatening damage to the liver over many years. It invades liver cells, causing inflammation, swelling, dysfunction, and eventual organ damage.
Common Cause
Hepatitis C is caused by the hepatitis C virus and rarely spreads through sexual contact. Hepatitis C is not contracted through kissing, sneezing, coughing, and sharing objects. A person can transmit the virus to someone else through blood-to-blood contact. The virus can be described as acute or chronic.
- Acute hepatitis C occurs within the first six months after someone is exposed to the hepatitis C virus. Hepatitis C can be a short-term illness, but acute infection leads to chronic infection for most people.
Chronic hepatitis C can be a lifelong infection if left untreated. Chronic hepatitis C can cause serious health problems, including liver damage, cirrhosis (liver scarring), liver cancer, and even death.
Symptoms
The symptoms of Hepatitis B and Hepatitis C are very much alike. The incubation period ranges from 2 weeks to 6 months. Most people do not exhibit symptoms, while some may exhibit:
- Fever
- Fatigue
- Reduced appetite
- Nausea
- Vomiting
- Abdominal pain
- Dark urine
- Pale feces
- Joint pain
- Jaundice (yellowing of the skin and the whites of the eyes)
Treatment
New infection with HCV does not always require treatment, as the immune response in some people will clear the infection. However, when HCV infection becomes chronic, treatment is necessary. It can be treated with medicines that stop the virus from multiplying inside the body. Current treatments usually involve just 8–12 weeks of pills or injections and cure most people with few side effects. In addition to this, regular checkups are essential to reduce the advancement of liver disease, including liver cancer.
But it’s essential to be aware that you will not be immune to the infection and should take steps to reduce your risk of becoming infected again.
Prevention
-
There is no vaccination to prevent hepatitis C. The best way to avoid it is to avoid exposure to blood that may contain hepatitis C.
- Never share needles, syringes, prevent and other injecting equipment
- Avoid contact with other people’s body fluids
- Always use condoms, gloves, or dental dams during sex if blood may be present.
- Never share personal items such as razors, toothbrushes, combs, and nail clippers.
Human Immunodeficiency Virus (HIV)
Human Immunodeficiency Virus (HIV) is a virus that attacks cells that help the body fight infection, making a person more vulnerable to other infections and diseases. If left untreated, it may lead to Acquired Immunodeficiency Syndrome (AIDS). AIDS is the late stage of HIV infection that occurs when the body’s immune system is badly damaged because of the virus.
There are three stages infected people go through if they don’t get treated early on Acute, Chronic, and AIDS. Symptoms range from flu to no signs to severe infections depending on the stage.
Common Cause
HIV infection in humans came from a type of chimpanzee in Central Africa. The virus was probably passed to humans when humans hunted these chimpanzees for meat and contracted their infected blood.
HIV can be transmitted through the infected human liquids, through unprotected sex of any type, through the infected needles for drugs injection, as well as the instruments for tattooing and from mother to child.
It is spread by contact with certain bodily fluids of a person with HIV, most commonly during unprotected sex (sex without a condom or HIV medicine to prevent or treat HIV) or through sharing injection drug equipment.
Symptoms
Some people get symptoms similar to the flu within 2 to 4 weeks after infection and may last for a few days to several weeks. Other possible symptoms include
- Fever
- Chills
- Rash
- Night sweats
- Muscle aches
- Sore throat
- Fatigue
- Swollen lymph nodes
- Mouth ulcers
Treatment
Once you get HIV, you have it for life. However, it can be controlled by a combination of medications to enable infected people to live long and healthy lives and prevent transmitting to their sexual partners.
It can be managed by treatment regimens composed of a combination of three or more antiretroviral (ARV) drugs. It does not cure HIV infection but highly suppresses viral replication within a person's body and allows an individual's immune system recovery to strengthen and regain the capacity to fight off opportunistic infections and some cancers.
Prevention
-
You can limit your exposure by:
- Male and female condom use
- Testing and counseling for HIV and STIs
- Use of antiretroviral drugs (ARVs) for prevention
- Prevent transmission from mother to baby by following doctors orders